Screening for Breast Cancer
Breast exams, either from a medical provider or self-exams, are no longer recommended for women at average risk for breast cancer. Women at high risk – because of family history, a breast condition, or another reason – need to begin screening earlier and/or more often. Talk to your doctor to be sure.
Age 20’s:
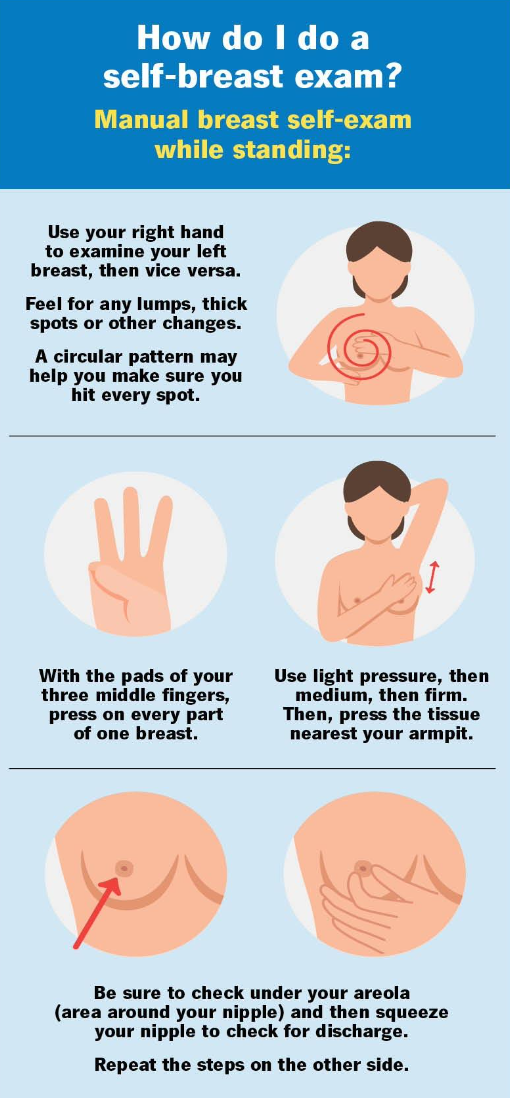
From the age of 20, women should know their family history of breast cancer and it is good to do a breast self- examination monthly in order to get to know your own breasts. Examine your breasts one week after your period ends. This way you will detect any changes in your breasts more easily.
Age 30’s:
Women over 30 should know their family history of breast cancer and can do a breast self- examination monthly. It is recommended to have a breast assessment by a health professional every three years to determine risk profile and need for imaging tests. If you have a Mirena IUCD, please discuss screening with your doctor.
Age 40’s:
Breast cancer treatments and technology have improved dramatically in the past few decades. It is useful to do a breast self-examination monthly. A mammogram is a low dose X-ray of your breasts. It can detect very small lesions which are not palpable but can be seen with imaging. This is the most important component and still the gold standard of early detection. A breast ultrasound will often be added to this and in specific cases a breast MRI might be recommended.
Women between 40 and 44 have the option to start screening with a mammogram every year. Women with an average risk of breast cancer, which are most women, should begin yearly mammograms at age 45-54. At age 55 and older, women should have mammograms every other year, although women who want to keep having yearly mammograms should be able to do so.
Definition of average risk:
- No personal history of breast cancer
- No strong family history of breast cancer
- No genetic mutation known to increase risk of breast cancer (such as BRCA gene)
- No chest radiation therapy before the age of 30
Definition of high risk:
- A lifetime risk of breast cancer of about 20% to 25% or greater, according to risk assessment tools that are based mainly on family history
- A known BRCA1 or BRCA2 gene mutation (based on having had genetic testing)
- A first-degree relative (parent, brother, sister, or child) with a BRCA1 or BRCA2 gene mutation, and have not had genetic testing themselves
- Had radiation therapy to the chest before they were 30 years old
- Have Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome, or have first-degree relatives with one of these syndromes