Hysteroscopy – Procedure and Recovery Information
What is hysteroscopy?
It is a procedure that involves examining the inside of your uterus (womb). This is done by passing a thin telescope-like device, called a hysteroscope, that is fitted with a small camera through the neck of your womb (cervix). The healthcare professional doing the procedure can then see whether there are any problems inside your uterus that may need further investigation or treatment.
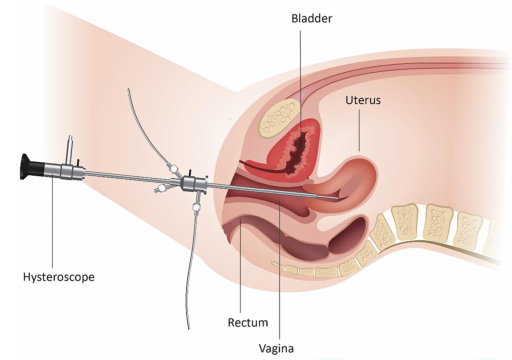
Why have I been recommended for a hysteroscopy?
This procedure may have been recommended for any of the following reasons:
- bleeding after the menopause (postmenopausal bleeding)
- very heavy periods
- bleeding between periods
- irregular bleeding while on hormonal treatment
- removal of a coil when the threads are not visible at the cervix
- fertility concerns
- following a miscarriage
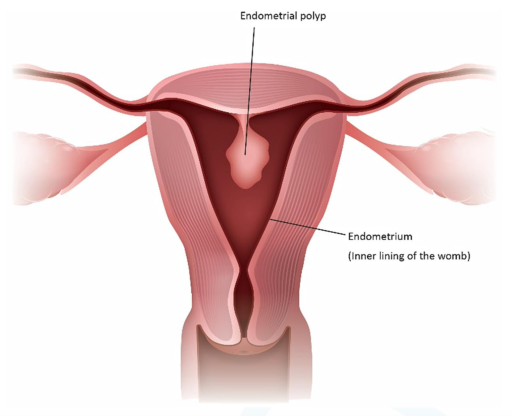
- to investigate something seen inside the uterus on an ultrasound scan, such as an endometrial polyp or fibroid.
It may be possible for a minor procedure to be done at the same visit, such as:
Endometrial biopsy – taking a sample from the lining of the uterus. This can be done through the hysteroscope.
Polyp removal – a polyp inside the uterus is a tag that looks like a small grape, sometimes on a stalk. Polyps are formed as a result of overgrowth of the lining of the uterus.
Fibroid removal – fibroids are growths in the muscle of the uterus that are non-cancerous(benign). They can sometimes bulge like a polyp into the lining of your uterus and your doctor may advise removal to help with your symptoms.
IUCD – Insertion of a hormone-releasing intrauterine device (for example, Mirena®).
Removal – IUCD removal from the uterus when the threads are not visible.
Do I need to use contraception?
The procedure must not be performed if there is any chance that you are pregnant. To avoid this possibility, it is important to use contraception or avoid sex between your last period and your appointment. You may be offered a urine pregnancy test on arrival at your appointment.
Can I still have an outpatient hysteroscopy if I’m bleeding?
It is best to keep the appointment. Sometimes it can be difficult to do the test if you are bleeding heavily. If you have any concerns, please ring and speak to your healthcare professional.
The procedure
A hysteroscope is passed through the cervix to give a clear view of the inside of your uterus. No cuts are needed. Fluid (saline solution) is used to help see the inner lining of your uterus and you will feel wet as the fluid trickles back out. If no problems are found, the actual procedure will only take about 10–15 minutes. Sometimes, a biopsy (small sample) from the lining of your uterus may be taken and sent to the laboratory for examination. The biopsy can be painful, but the pain should not last long. If a fibroid or polyp is found, it can sometimes be removed at the same time by using additional instruments. Photographs of the findings inside your uterus are often taken and kept in your healthcare notes.
What are the possible risks with hysteroscopy?
Pain during or after is usually mild and similar to period pain. Simple pain relief medications can help. On occasion, women may experience severe pain.
Feeling or being sick or fainting can affect a small number of women. However, these symptoms usually settle quickly. Let your doctor know if you are feeling unwell during or straight after the procedure.
Bleeding is usually very mild and is lighter than a period, settling within a few days. It is recommended that you use sanitary towels, not tampons. If the bleeding does not settle and gets worse, contact your doctor or nearest emergency department.
Infection is uncommon (1 in 400 women). It may appear as a smelly discharge, fever or severe pain in the tummy. If you develop any of these symptoms, contact your doctor urgently.
Failed/unsuccessful hysteroscopy occurs if it is not possible to pass the hysteroscope inside your uterus. Usually this happens when the cervix is tightly ‘closed’ or scarred. If this happens, your doctor will discuss alternative options with you.
Damage to the wall of the uterus (uterine perforation) – rarely, a small hole is accidentally made in the wall of the uterus. This could also cause damage to nearby tissues. This happens in fewer than 1 in 1000 diagnostic hysteroscopy procedures, but is slightly more common if someone has a polyp or fibroid removed at the same time. It may mean that you have to stay in hospital overnight. Usually, nothing more needs to be done, but you may need a further operation to repair the hole.
How will I feel afterwards?
You may get some period-like pain for 1–2 days. You may also have some spotting or fresh (bright red) bleeding that may last up to 1 week. These symptoms usually settle very quickly. Most women feel able to go back to their normal activities on the same day.
You can shower as normal.
Normal physical activity and sex can be resumed when any bleeding and discomfort has settled.
If needed, you can take pain relief such as 400 mg of ibuprofen every 8 hours or 1 gram of paracetamol every 4 hours, or your usual period pain tablets.
If your pain is not controlled with the above medication, you should contact your doctor or nearest emergency department.

