LLETZ and Colposcopy Information
What is a LLETZ?
A LLETZ stands for large loop excision of the transformation zone. This procedure will remove a small segment of the cervix (the lower part of your womb or uterus).
What is a cone Biopsy?
A cone biopsy is a less common surgical procedure where a cone-shaped or cylinder-shaped piece of the cervix is removed.
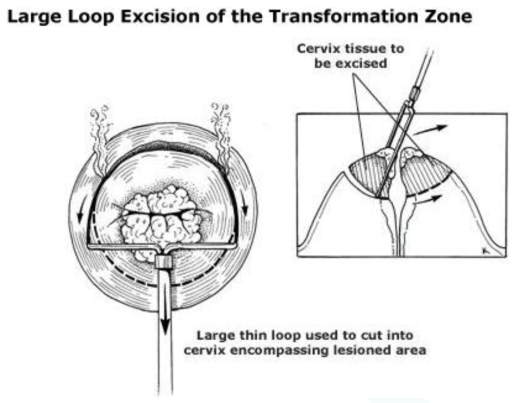
Why are they performed?
These procedures are performed for the diagnosis and treatment of pre-cancerous cells of the cervix. You should have a clear understanding of your reason for this surgery – if not, please ask your doctor.
What are the alternatives?
A LLETZ or cone biopsy are recommended in order to treat pre-cancer cells. If you choose not to undergo treatment, there is a strong likelihood that these changes would progress to cancer over some years. If you did not have treatment, it would be essential for you to have ongoing close follow-up in the colposcopy clinic.
How are they performed?
The procedure is usually performed under a general anaesthetic. The cervix is examined using a special microscope called a colposcope (in the same way as you were examined in the clinic). A fine wire loop charged with electricity is used to shave away the abnormal tissue from the cervix. Because the procedure is so exact, and the loop very thin, very little damage is done to the tissue surrounding the area that needs to be removed. The procedure allows for the blood vessels surrounding the area to be sealed.
A cone biopsy is more commonly performed under a general anaesthetic. The abnormal cells are often cut out with a knife. Dissolvable sutures are used to stop the bleeding. Both procedures take approximately fifteen minutes or more.
What the risks of undergoing this procedure?
Although the risks associated with a LLETZ procedure or a cone biopsy are low, you should be aware that every surgical procedure has some risk.
There are some specific risks to be aware of in relation to this operation:
- Excessive bleeding from the cervix, which may need blood transfusion or further surgery, either initially or within weeks of the procedure.
- Infection may be introduced into the cervix, uterus, tubes or abdomen. This may require treatment with antibiotics.
- Sometimes not all of the abnormal tissue is completely removed, requiring further surgery.
- Uncommonly the wire might cause an injury to the surrounding vaginal tissue.
- Uncommonly, the cervix may be weakened by this procedure resulting in a slight increase in the further pregnancy risk of a late miscarriage or preterm birth.
- Rarely the cervix may be damaged and narrowed leading to painful periods, difficulty in performing adequate pap smears, or problems in the progress of a future labour.
What should I do before the procedure?
Follow the instructions given to you for your surgery paperwork and register with the hospital
- You should continue your regular medication, unless advised otherwise.
- Stop smoking
- Should you develop an illness prior to your surgery, please contact us
- Should you end up with your period the day you are due for your LLETZ you do not need to cancel your surgery, you can still proceed.
What should I do on the day of the procedure?
- Arrive to hospital as per your surgery confirmation time.
- You should have fasted as per your surgery confirmation.
What should I expect after the procedure?
- You should be able to leave the hospital that day.
- The hospital will provide you with discharge information and medication if required.
- You may use paracetamol as required.
- You should expect a bloody vaginal discharge for several days after the procedure, which should settle within one to two weeks.
- A clear discharge may persist for up to six seeks. You should be able to return to work the following day, but may require more time off work.
- Follow up appointments are very important to ensure that all of the abnormal cells have been removed. You will have a post-operative appointment arranged for you.
- After discharge from the hospital, you should eat and drink normally, remain mobile, use sanitary pads (not tampons) if required and shower normally (in preference to bathing).
You should NOT have intercourse for six weeks. - If you have any fevers or feeling unwell, offensive vaginal discharge or heavy bleeding please contact your doctor or present to the casualty unit at the hospital.